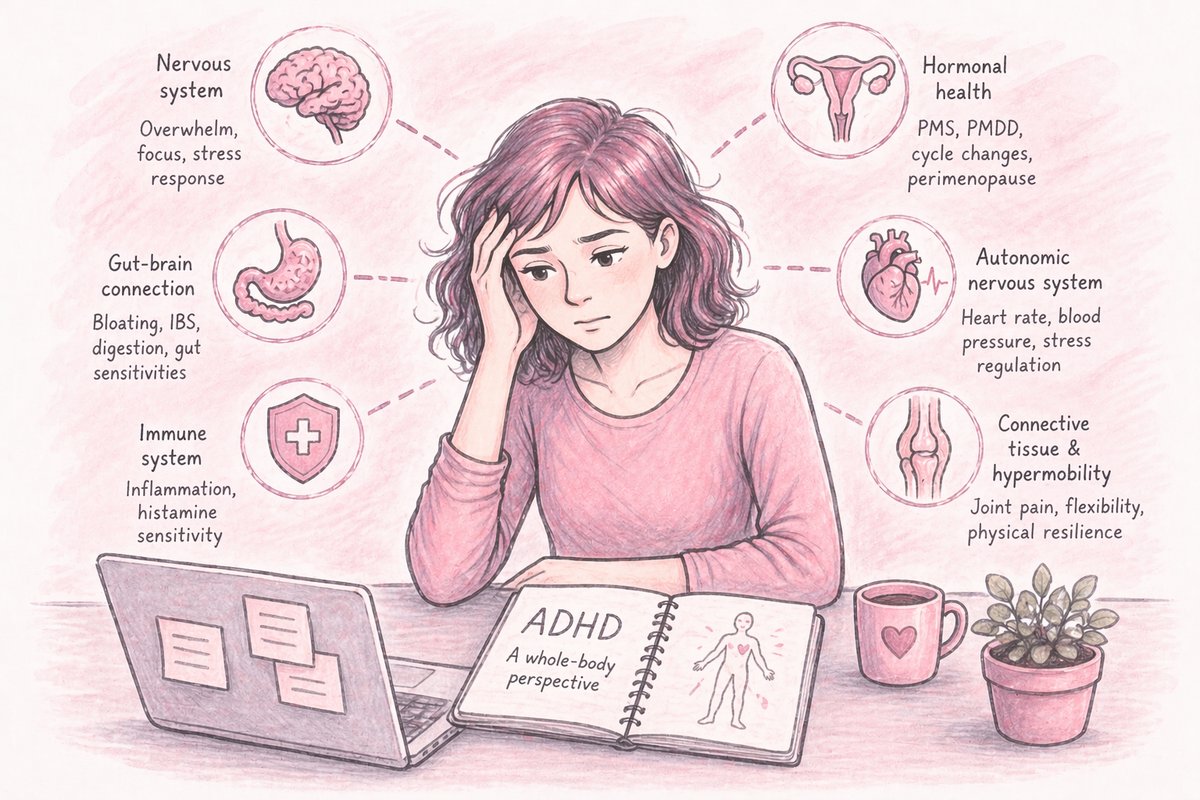
ADHD Is Not Just in the Brain: A Whole-Body Perspective in Women
People are becoming much more aware of Attention Deficit Hyperactivity Disorder (ADHD) in women. For many years, ADHD was mostly linked to boys and the more obvious hyperactivity often seen in classrooms. Now, that view is shifting. More women are being diagnosed as adults, which is helping us better understand the many ways ADHD can present.
What I Notice in Practice
As a nutritional therapist, I often see women with ADHD in my practice. Most do not come in because of difficulty with focus or attention. Instead, they are looking for support with low energy, hormonal concerns, digestion, sleep, or a general sense that something is not quite right.
Over time, I have noticed a consistent pattern. Alongside common ADHD symptoms such as feeling overwhelmed, difficulty focusing, and being mentally alert but physically tired, many women also report:
- Hormone-related mood changes or severe PMS
- Chronic fatigue or persistently low energy
- Sleep disturbances
- Digestive symptoms such as bloating or IBS-type symptoms, often linked to gut-brain and nervous system dysregulation
- Joint hypermobility or ongoing musculoskeletal pain
- Dizziness or lightheadedness
- Food sensitivities or histamine-related symptoms
- Painful or heavy periods, including conditions such as endometriosis
These symptoms are often addressed individually. In practice, however, they rarely occur in isolation. They tend to cluster together in ways that suggest underlying connections.
ADHD and the Body
ADHD is officially classified as a neurodevelopmental condition, and that remains an important part of how it is understood. However, both emerging research and clinical observation suggest that, for many women, ADHD may involve more than just brain-based processes.
It often appears to interact with multiple body systems, including:
- The nervous system, which influences attention, stress responses, energy regulation, and gut-brain signalling
- Hormonal systems, particularly sensitivity to changes in oestrogen and progesterone
- The immune system, including possible links with inflammation and histamine
- The autonomic nervous system, which regulates heart rate, blood pressure, and the stress response
- Connective tissue, particularly in individuals with joint hypermobility
I also frequently observe overlap with patterns seen in hypermobility spectrum presentations and symptoms associated with Mast Cell Activation Syndrome (MCAS), although research in this area is still evolving.
This does not suggest that ADHD directly causes these conditions. However, it raises an important question: whether there are shared underlying mechanisms contributing to these patterns.
Taken together, this points towards ADHD in women involving not only neurological processes, but also broader neuroendocrine, immune, and regulatory systems.
Hormones and Symptom Changes
One area that stands out in both research and practice is the relationship between ADHD and hormonal health. Many women notice that their ADHD symptoms fluctuate across the menstrual cycle, particularly during the luteal phase.
Some also experience more pronounced premenstrual symptoms, including low mood, irritability, and reduced motivation, sometimes consistent with Premenstrual Dysphoric Disorder (PMDD).
Hormonal transitions such as puberty, the postpartum period, and perimenopause can further influence how ADHD presents. This may help explain why many women are not diagnosed until later in life, particularly when hormonal shifts and increasing life demands make previously effective coping strategies and masking more difficult to sustain.
Why ADHD in Women Is Often Missed
There are several reasons why ADHD in women has historically been overlooked. Women are more likely to present with internalised symptoms such as anxiety, low mood, or chronic overwhelm, rather than more visible hyperactivity.
In addition, many women develop strong coping strategies and masking behaviours, which can make ADHD less obvious. Hormonal fluctuations can also alter how symptoms present over time, further complicating the picture.
As a result, many women are initially diagnosed with anxiety or depression, with ADHD only being considered later. This is beginning to change, but there is still much to learn about how ADHD affects women specifically.
A More Integrated View
Rather than viewing ADHD solely as a brain-based condition, it may be more accurate to consider it as a whole-person neurotype that interacts with multiple systems in the body.
For some women, this may include hormonal sensitivity, nervous system dysregulation, immune or inflammatory tendencies, and differences in connective tissue or physical resilience.
This perspective does not replace conventional ADHD care. However, it allows for a more personalised and comprehensive approach, particularly for women whose symptoms do not fit neatly into a single category.
Final Thoughts
We are still learning about the full complexity of ADHD in women. What is becoming increasingly clear is that, for many women, the experience extends beyond attention and focus alone.
Recognising these broader patterns can be both validating and clinically useful. It also allows for more personalised and effective support, which is often where the greatest improvements are seen.
If you are a woman with ADHD and feel your symptoms go beyond focus or attention, you are not alone. If you would like support with energy, hormones, digestion, or a more whole-body approach to ADHD, I would be very happy to help. You can book a free 20-minute discovery call here to explore your symptoms and see whether this approach feels like the right fit for you.
Karine x